
Physical Therapy for Foot and Ankle
The foot and ankle joints are major weight-bearing joints in your body and the ankle joint is the most commonly injured joint in your body. There are 28 bones and 33 joints, as well as many muscles, tendons, nerves, and ligaments in your foot. The foot and ankle work together to provide flexibility and stability to allow you to walk, run, balance, and many other weight-bearing activities.
At least 80% of people have foot problems, which can cause stress on other joints in your lower extremities. 1 An estimated 2 million people a year are treated for ankle sprains, strains, and fractures.2 Thirty to seventy percent of people will experience chronic ankle instability after an injury.3 There are many conditions of the foot and ankle that a physical therapist can help you with, including recovering from an injury, preventing injuries, help you with foot and/or ankle pain, and even help with balance.
Ankle sprains are one of the most common injuries of the foot and ankle and is usually accompanied by pain and swelling. They often occur during walking on uneven ground, running, or jumping. Although this type of injury often improves quickly, more than 70% of people continue to have problems and 80% will sprain their ankles again. Therefore it is important to seek treatment. A physical therapist can help restore normal joint movement with manual techniques as well as give you a supervised exercise program to improve mobility and prevent re-injury. One study showed that patients treated by a physical therapist had superior results compared to those that were given exercises to perform on their own. Benefits from being treated by a physical therapist include less pain and an “improved ability to perform daily activities and return to sport.”4
“A physical therapist can help restore normal joint movement with manual techniques as well as give you a supervised exercise program to improve mobility and prevent re-injury.”
Plantar fasciitis is another common condition that can be treated by a physical therapist. This condition is often characterized by a sharp stabbing pain near the heel of the foot and often occurs when first getting out of bed in the morning, after long periods of sitting, and with prolonged standing.5 The plantar fascia is a thick band of tissue that extends from the bottom of the heel to the toes. It is thought that this tissue becomes inflamed, but there is some controversy on which tissue is actually affected. Risk factors for plantar fasciitis include age (more common between 40 – 60 years old), certain types of exercise (including long-distance running), obesity, occupations that require prolonged standing, and foot mechanics. Often those with plantar fasciitis also present with a flat foot or a high arch.
Another condition that causes heel pain is Achilles tendinopathy or tendonitis. The Achilles tendon connects your calf muscle to the heel bone (the calcaneus) and it is the largest tendon in your body. This tendon can become swollen and painful due to degenerative changes. Achilles tendinopathy can happen in both inactive and physically active people; however, it is more common in those who are active. It is commonly found in those who play racquet sports and runners6 and is characterized by stiffness and pain in the Achilles tendon in the morning, swelling in the back of the ankle and pain that gets worse with increased activity, thickening of the tendon, and/or increased pain the day after increased activity. If you hear a pop, you may have partially or completely ruptured the Achilles tendon.

Posterior tibialis tendon dysfunction is the most common cause of “flatfoot” and occurs when there are degenerative changes in the posterior tibialis tendon.7 The posterior tibialis helps to support the arch of the foot during standing and walking. With this dysfunction, the arch of your foot drops and your foot may start to turn outwards. This can cause pain and swelling on the inside of the foot and ankle. Without treatment, this condition tends to get worse and can cause deformities in the foot and ankle. Fractures can occur in the ankle and foot.
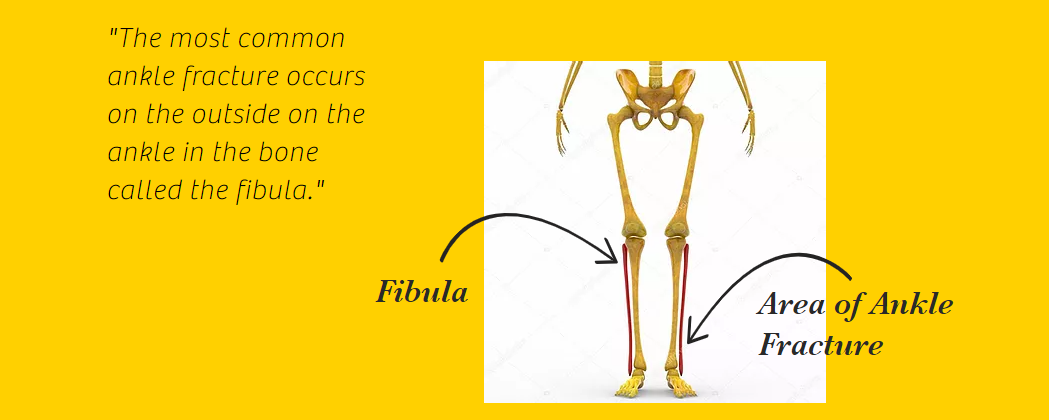
The most common ankle fracture occurs on the outside of the ankle in the bone called the fibula. Fractures can also occur on the inside of the ankle. These fractures are characterized by pain, swelling, deformity, and inability to put weight on that foot. Some fractures require surgery, while others only require immobilization in a boot or cast. A stress fracture is a small break in the bone, usually caused by overuse. The most common stress fractures are in the second and third metatarsals, but can also be found in the heel and the navicular (a bone in the top of the foot). Symptoms may include minor pain or weakness where the fracture is located, deep pain in the foot, ankle, or toe, pain during normal activity, decrease in pain with rest, and increased pain after increased activity.8
Bursae are small fluid-filled sacs located all over your body, including your foot, that help to decrease friction. These fluid-filled sacs can become irritated from overuse and stress and lead to bursitis. Symptoms include pain and tenderness where the bursa is located, loss of motion, and swelling. Bursitis of the foot region is often found in patients with rheumatoid arthritis.9
Physical therapy can help with many conditions in the foot or ankle. Whatever the issue may be, your therapist will first perform an evaluation that will include assessing the way you walk, your standing posture, range of motion, balance, and strength. Your therapist will also make sure to assess your low back and other joints in your legs to address other conditions that may be contributing to your foot problem. Often after surgery, joints can become hypomobile, or stiff, and muscles can become weak due to lack of use and movement. If there are joints that are hypomobile or muscles that are tight or weak, your therapist will use manual techniques and exercises to get these parts moving and get them stronger. If you have hypermobile joints, or more than usual flexibility, your therapist will help you to get more stability. Your therapist is here to help you back to recovery so you can once again do the things you enjoy without pain, whether that is running a half marathon or simply standing.
-
- Kangas J, Dankaerts W, Staes F. New approach to the diagnosis and classification of chronic foot and ankle disorders: identifying motor control and movement impairments. Manual Therapy. 2011 Dec;16(6):522-30.
- Shah S, Blanchette CM, Noone J, Wikstrom EA. Prevalence and burden of ankle injuries in North Carolina emergency departments. Value in Health. 2015;18(3):A250.
- Medina McKeon JM, Hoch MC. The ankle-joint complex: A kinesiologic approach to lateral ankle sprains. Journal of Athletic Training. 2019;54(6):589-602.
- Cleland JA, Mintken PE, McDevitt A, Bieniek ML, Carpenter KJ, Kulp K, Whitman JM. Manual Physical Therapy and Exercise Versus Supervised Home exercise in the Management of Patients with Inversion Ankle Sprain: A Multicenter Randomized Clinical Trial. Journal of Orthopedic Sports Physical Therapy. 2013;43(7):443-455.
- Thompson JV, Saini SS, Reb CW, Daniel JN. Diagnosis and management of plantar fasciitis. Journal of the American Osteopathic Association. 2014 Dec;114(12):900-6.
- Maffulli N, Sharma P, & Luscombe K. Achilles tendinopathy: aetiology and management. Journal of the Royal Society of Medicine. 2004 Oct; 97(10): 472–476.
- Bubra PS, Keighley G, Rateesh S, & Carmody D. Posterior Tibial Tendon Dysfunction: An Overlooked Cause of Foot Deformity. Journal of Family Medicine and Primary Care. 2015 Jan-Mar; 4(1): 26–29.
- American Academy of Orthopaedic Surgeons: Stress Fractures of the Foot and Ankle
- Hammer HB, Kvien TK, Terslev L. Intermetatarsal bursitis is frequent in patients with established rheumatoid arthritis and is associated with anti-cyclic citrullinated peptide and rheumatoid factor. RMD Open. 2019;5(2):e001076.
BY: livetomovept
Massage Therapy
COMMENTS: 7 Comments





